In April 2023, CMS released a set of proposed rules surrounding access, financing and quality of Medicaid Managed Care programs. While the rules have yet to be finalized, IPRO has analyzed the proposals and based on nearly 35 years of experience as a Medicaid External Quality Review contractor, is poised to assist states with compliance.
 Since 1989, IPRO has been working with state Medicaid agencies to enhance the value of healthcare services provided to the Medicaid managed care population. Our work as an External Quality Review Organization (EQRO) predates the issuance of the federal external quality review protocols by 15 years, making IPRO among the most experienced and qualified EQROs in the nation.
Since 1989, IPRO has been working with state Medicaid agencies to enhance the value of healthcare services provided to the Medicaid managed care population. Our work as an External Quality Review Organization (EQRO) predates the issuance of the federal external quality review protocols by 15 years, making IPRO among the most experienced and qualified EQROs in the nation.
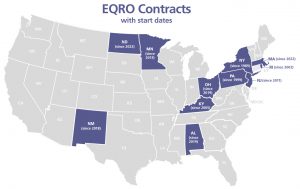
We understand that your state has unique demographics, issues, interests, and ways of working that drive your EQR program goals. IPRO works with states of all sizes, from New York, with 4.7 million MMC enrollees (the second largest cohort in the nation), to North Dakota, with fewer than 22,000 enrollees. Our approach emphasizes collaboration with our clients to gain insight into their particular Medicaid populations and objectives so that we can tailor our solutions to meet their needs.
Read About IPRO’s EQRO Experience
IPRO is monitoring CMS’ proposed Medicaid Managed Care rule changes regarding access, quality and finance. Join our mailing list to receive updates on the proposed changes and information on compliance.