FROM: Theodore O. Will, FACHE /s/ Chief Executive Officer
DATE: July 1, 2014
RE: UPDATE IN REGARD TO 11TH SCOPE OF WORK (SOW) QUALITY IMPROVEMENT ORGANIZATION (QIO) PROGRAM AND CASE REVIEW/BENEFICIARY AND FAMILY-CENTERED CARE ACTIVITIES
IPRO CONTACT: Andrea Goldstein, Vice President, Medicare/Federal Health Care Assessment, 516-209-5364
The purpose of this Memorandum is to provide an update in regard to the changes that the Centers for Medicare and Medicaid Services (CMS) has made to the Quality Improvement Organization (QIO) case review/beneficiary and family-centered care program. These changes will occur on August 1, 2014.
Suggested Distribution List:
- Medical Director
- Compliance Officer
- Director of Utilization Management
- Quality Improvement
- Director of Health Information Management
- Risk Manager
- Credentialing Office
High Level QIO Program Transition Synopsis:
- CMS has restructured the QIO Program from its historical 53 contracts, in which each QIO performs both case review and quality improvement support for each state or territory to a regional structure for case review and an industry-determined service structure for quality improvement initiatives.
- In the new structure, case review and quality improvement functions are performed by different contractors, the contract periods are extended from 3 to 5 years, and there is enhanced focus on learning, collaboration, and the dissemination of best practices.
- One group of QIOs will handle complaints while another group will provide technical assistance to support providers and suppliers. QIOs will have new skills in the area transforming practices, employing lean methodologies, assisting with value based purchasing programs and developing innovative approaches to quality improvement.
- The Beneficiary and Family Centered Care Quality Improvement Organizations (BFCC-QIO) will manage all beneficiary complaints and quality of care reviews to ensure consistency in the review process while taking into consideration local factors important to beneficiaries and their families.
- Quality Innovation Network (QIN) QIOs will be responsible for working with providers and the community on multiple, data-driven quality initiatives to improve patient safety, reduce harm, and improve clinical care at their local and regional levels.
Case Review/Beneficiary & Family Centered Care:
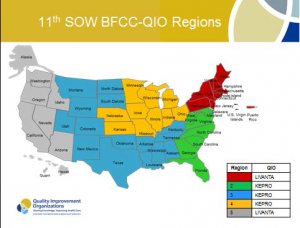
As you may recall, on May 9, 2014, CMS launched its first phase of the transition by awarding the QIO Program Beneficiary and Family Centered Care Quality Improvement Organization (BFCC-QIO) contracts. As shown in the BFCC-QIO Regional Map, below, BFCC-QIO Regions 1&5 have been awarded to LIVANTA, and Regions 2, 3, & 4 to KePRO. This means that:
- On August 1, 2014, all IPRO current (i.e., in process) and future case review activities, including but not limited to beneficiary complaints/quality review case work and appeals will be conducted by Livanta.
- IPRO is making every effort to ensure a seamless transition to Livanta with no disruption in review services for all cases currently under review or that will be in process on July 31, 2014.
As the incoming BFCC-QIO, Livanta is expected to have knowledge of the culture, practices, and healthcare improvement needs of the communities where it will conduct work and will apply that knowledge to its case review activities. CMS has stated that:
- The redesign of the QIO Program will not lessen the contractual obligations of the QIOs to meet the local needs of their constituents, regardless of geographic factors that are unique to care in their service areas.
- CMS will continue to monitor and evaluate QIO contractors based on their performance in each state to ensure that contract responsibilities are fulfilled
- IPRO will continue to provide Case Review Transition updates as information is received from Livanta and CMS. In addition, more information on the QIO Program can be found at QIOProgram.org. In the interim, should you have any questions in regard to this memorandum, please contact Andrea Goldstein at 516-209-5364.