How come so many Americans feel so badly about their healthcare system?
 This question came to mind during presentations by Harvard economist David Cutler, PhD and Former CMS Administrator Donald Berwick, MD, MPP at an online symposium held February 12, 2015, sponsored by the Institute for Healthcare Improvement.
This question came to mind during presentations by Harvard economist David Cutler, PhD and Former CMS Administrator Donald Berwick, MD, MPP at an online symposium held February 12, 2015, sponsored by the Institute for Healthcare Improvement.
Cutler’s first four slides illustrate startling, across-the-board findings that might seem preposterous, except that they’re true:
(1) the percentage of U.S. adults without health insurance has declined sharply from a high of 18 percent in late 2013 to a low of 12.9 percent at the end of 20014 (Gallup),
(2) the number of adults who report they’re not getting needed care because of cost concerns declined last year for the first time since 2003 (Commonwealth),
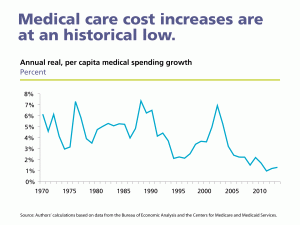
(3) medical cost increases are at a 40-year low, with annual real, per capita spending increasing by as little as 1 percent in 2010 (Cutler’s calculation with Bureau of Economic Analysis and CMS data),
(4) central line-associated bloodstream infection rates at hospitals are 46 percent lower compared to a national baseline (CDC, 2015).
Surely findings like these– if more widely known– would have a positive affect on the way Americans think about their healthcare delivery system. But more often than not, what we hear from Washington DC is a steady din of rhetoric that has the depressing effect of debasing discussion and obscuring understanding of our own recent history.
Figure 1-Medical care cost increases are at an historical low
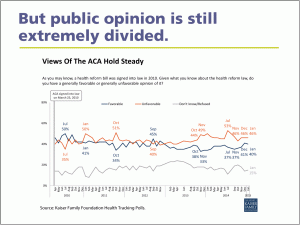
Indeed, the only slide that Professor Cutler offered that didn’t show dramatic change was an opinion slide from the Kaiser Family Foundation, which tracks Americans views of the Affordable Care Act. That slide finds rates of favorable/unfavorable at about the same levels in 2015 that they were in 2010. In other words, opinions can harden into convictions to the point where nothing else really matters.
Figure 2-Views of the ACA Hold Steady
While Berwick echoes Cutler in seeing recent, demonstrable progress in addressing the triple aim of better health, better healthcare and reduced cost (Berwick’s own formulation, which he attributes to colleagues at IHI, where he is President Emeritus), he also finds plenty of room for improvement, arguing that 30 percent to 40 percent of total effort in the U.S. healthcare system is “of no value to patients.”
And both experts worry about the increasing burden of employee cost-sharing, which could over time erode much of the real progress we’re making in improving access, quality and cost for the large number of Americans who continue to obtain coverage from their employers.
But maybe it’s time to recognize that some of the news is actually quite good.
Spencer Vibbert is IPRO’s Vice President for External Affairs
For more information on The Ups and Downs of Health Care Costs and Reform, visit IHI.org/WIHI
Graphics. Cambridge, Massachusetts: Institute for Healthcare Improvement; 2015 (available on www.IHI.org)